Non-surgical Treatments
These will be
Pain-relieving Medication
 Initially, the simplest treatment is for you to take analgesia, or pain relieving medication. Some patients with heart issues, asthma, stomach problems or kidney problems may not be able to take an anti-inflammatory medication a it can make these worse. Dr. Thornton-Bott will review your medical history and discuss this with you.
Initially, the simplest treatment is for you to take analgesia, or pain relieving medication. Some patients with heart issues, asthma, stomach problems or kidney problems may not be able to take an anti-inflammatory medication a it can make these worse. Dr. Thornton-Bott will review your medical history and discuss this with you.
If you are taking regular simple pain medication and still have pain, then you may require stronger medication. Some patients are scared they will get addicted to these stronger medications, but if taken appropriately for severe pain, this is unlikely, and all options will be discussed so you can make an informed decision.
Physiotherapy
 Exercise therapy has been shown to help with both pain and stiffness in patients with osteoarthritis. Sometimes, patients who have been booked for a joint replacement get such a good result from physiotherapy that they no longer require the operation, or at least the operation can be delayed for months or even years!
Exercise therapy has been shown to help with both pain and stiffness in patients with osteoarthritis. Sometimes, patients who have been booked for a joint replacement get such a good result from physiotherapy that they no longer require the operation, or at least the operation can be delayed for months or even years!
The exercise regimen will be developed specifically for you by our qualified Physiotherapists who have extensive experience in patients with OA of the hip or knee. Some patients can manage many exercises and others only a few. The aim is to maintain a good range of motion and ensure you are walking as well as you can and as comfortably as you can. Simple measures will be discussed with you such as pain free ways to climb stairs and get out of a chair. These may seem obvious, but just by changing the way in which you do these everyday activities may significantly reduce your pain.
Weight Loss
 When you put your left foot on the ground and swing your right foot forward during walking, you can put 2-3 times body weight through your hip and knee.
When you put your left foot on the ground and swing your right foot forward during walking, you can put 2-3 times body weight through your hip and knee.
This is simple mechanics. The knee and hip are not in the centre of the body, but are a distance away from your centre of gravity, hence body weight multiplied by distance of the hip or knee from the centre of gravity creates a force that is greater then the body weight. (See the fig below) When running, these forces are higher, and when going up and down steps the forces are up to 5 times body weight.
Increased weight, and when excessive, obesity is a universal issue in the developed world. Not only can it cause significant medical problems such as early onset diabetes, it also puts a huge strain on your hips and knees. The articular cartilage resists the forces placed upon the joint, but if these forces are excessive the cartilage can become damaged and become arthritic. When you get arthritis, the increased weight increases the force in the joint and thus increases the pain.
Millions of years of evolution have created a skeleton in a woman of 160cm tall to have an ideal weight of around 55kg, giving her a Body Mass Index (BMI) of 21.5. As such, if you are a woman of 160 cm and weigh 80kg, you are putting up to 75kg (3x25) more through your hip or knee than it is designed to carry. You will have a BMI of 31.
Importantly, the reverse is also true, in that if you do weigh 80kg and are 160cm and lose weight, then for every 1kg you lose you will be taking 2-3 kg off your joints.
This is why weight loss in patients with osteoarthritis can have a huge impact on your pain. It is common for patients who have moderate OA of the hip or knee and successfully lose weight to also lose some or most of their pain.
It can feel very difficult to exercise because of the pain, but weight loss is also 80% of what you eat and 20% what you do. If you are unable to do any exercise, then weight loss is 100% of what you eat.
It is easy to say ‘Lose weight!’ and much harder to do it! There are many avenues and help that is available to patients who want to, or need to lose weight and Dr. Thornton-Bott can discuss these with you. We are here to help you.
If your arthritis is advanced, then weight loss will not change the need for surgery, such as joint replacement. However, losing weight will make the surgery easier, your risks lower and your rehabilitation easier.
Cortisone Injection
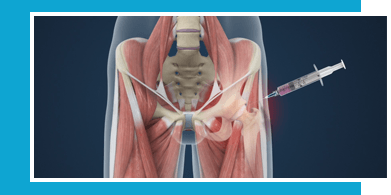 An aspect of osteoarthritis is inflammation. This is why you may get swelling of the knee, but also pain. Anti-inflammatory medications are good as a baseline but sometimes are not enough to keep the inflammation at bay. In these cases, a steroid injection can be beneficial. Corticosteroid is a potent anti-inflammatory and many patients with early to moderate OA will have a good result, with moderate or even complete pain relief. The benefits from a steroid infection can last from a few weeks up to a year in some cases. If the pain relief lasts for several months it can be repeated. However, in more severe OA, steroid injections are usually not beneficial, and if the benefits are short lived, the next best option will be surgery.
An aspect of osteoarthritis is inflammation. This is why you may get swelling of the knee, but also pain. Anti-inflammatory medications are good as a baseline but sometimes are not enough to keep the inflammation at bay. In these cases, a steroid injection can be beneficial. Corticosteroid is a potent anti-inflammatory and many patients with early to moderate OA will have a good result, with moderate or even complete pain relief. The benefits from a steroid infection can last from a few weeks up to a year in some cases. If the pain relief lasts for several months it can be repeated. However, in more severe OA, steroid injections are usually not beneficial, and if the benefits are short lived, the next best option will be surgery.
The steroid injection is a very simple injection that is performed by Dr. Thornton-Bott in his rooms when required into the knee. Because of the depth of the joint, steroid injections into the hip are performed with image guidance such as x-ray or low dose CT scan and therefore not in the rooms.













